Items filtered by date: October 2024
Causes and Types of Flat Feet
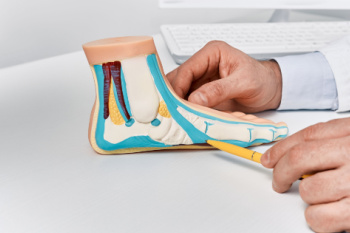
Flat feet, or pes planus, is a common condition where the arches of the feet are either low or completely absent, causing the soles to make full contact with the ground. The causes of flat feet can vary widely, including genetic predisposition, muscle imbalances, and injuries that affect the ligaments and tendons. In some cases, flat feet can develop during childhood as the arches form, while others may experience it as adults due to wear and tear or medical conditions. There are two primary types of flat feet, which are known as flexible and rigid. Flexible flat feet are characterized by arches that appear when sitting but flatten when standing, usually causing minimal discomfort. Rigid flat feet maintain a flat appearance regardless of position and can lead to pain and difficulty with movement. Flat feet can cause pain and discomfort. If you have this condition, iti is suggested that you consult a podiatrist who can offer you relief tips, and guide you on what type of shoes to wear.
Flatfoot is a condition many people suffer from. If you have flat feet, contact David K. Morris, DPM from Florida. Our doctor will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
- Pain around the heel or arch area
- Trouble standing on the tip toe
- Swelling around the inside of the ankle
- Flat look to one or both feet
- Having your shoes feel uneven when worn
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact our office located in Plantation, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Tips for Improving Your Balance

Improving balance is an important way to reduce the risk of falls, especially as people age. Foot-related issues such as nerve damage, weakened muscles, and joint problems can disrupt balance and increase the risk of injury. Exercises that focus on foot strength and flexibility are helpful in maintaining stability. Finding supportive footwear that fits well can also make a significant difference by providing a stable base. A podiatrist can assess any medical conditions that affect your feet, such as fallen arches or neuropathy. Custom orthotics, certain exercises, or assistive devices can help to improve your balance. Scheduling regular foot check-ups is a good way to detect early signs of issues that might contribute to instability. Making small changes, such as decluttering walkways and ensuring adequate lighting, can reduce hazards at home. If you have fallen and have injured your foot or ankle, or at risk for falling, it is suggested that you schedule an appointment with a podiatrist for an exam and treatment options.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with David K. Morris, DPM from Florida. Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact our office located in Plantation, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Facts About Cracked Heels
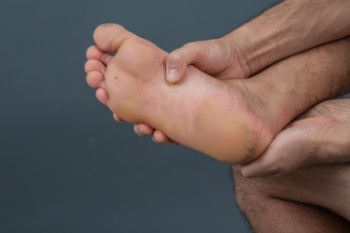
Cracked heels, also known as heel fissures, occur when the skin on the heels becomes dry and thickened, leading to painful splits. Several factors contribute to this condition. Excess weight can put additional pressure on the heels, promoting dryness and leading to cracks. Reduced skin elasticity, often due to aging or lack of moisture, makes the skin less resilient. Wearing inappropriate shoes, such as those lacking adequate support or cushioning, can worsen the problem by failing to protect the heels. Prolonged standing or walking on hard surfaces can also increase the risk of cracked heels, as this puts strain on the skin. Additionally, genetics may play a role in an individual's susceptibility to this condition. Cracked heels can be painful and may cause difficulty in completing daily activities. If you have developed cracked heels, it is strongly suggested that you consult a podiatrist who can successfully treat this problem, which may include prescribed medication.
Cracked heels are unsightly and can cause further damage to your shoes and feet. If you have any concerns, contact David K. Morris, DPM from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
Cracked heels appear unappealing and can make it harder for you walk around in sandals. Aside from looking unpleasant, cracked heels can also tear stockings, socks, and wear out your shoes. There are several methods to help restore a cracked heel and prevent further damage.
How Do You Get Them?
Dry skin is the number one culprit in creating cracked heels. Many athletes, walkers, joggers, and even swimmers suffer from cracked heels. Age and skin oil production play a role to getting cracked heels as well.
Promote Healing
Over the counter medicines can help, especially for those that need instant relief or who suffer from chronic dry feet.
Wear Socks – Wearing socks with medicated creams helps lock in moisture.
Moisturizers – Applying both day and night will help alleviate dryness which causes cracking.
Pumice Stones – These exfoliate and remove dead skin, which allows for smoother moisturizer application and better absorption into the skin.
Change in Diet
Eating healthy with a well-balanced diet will give the skin a fresh and radiant look. Your body responds to the kinds of food you ingest. Omega-3 fatty acids and zinc supplements can also revitalize skin tissue.
Most importantly, seek professional help if unsure how to proceed in treating cracked heels. A podiatrist will help you with any questions or information needed.
If you have any questions, please feel free to contact our office located in Plantation, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Heel Pain Can Be Treated!
Understanding Plantar Fibromatosis
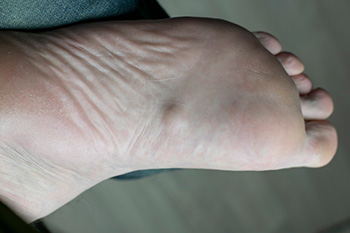
Plantar fibromatosis, also known as Ledderhose's disease, is the development of fibrous nodules in the plantar fascia, the connective tissue that runs along the bottom of the foot. These nodules can vary in size and may lead to discomfort or pain, particularly during activities such as walking or running. Common symptoms include noticeable lumps on the arch of the foot, localized tenderness, and a feeling of tightness in the affected area. While the exact cause of Ledderhose's disease remains unclear, genetic factors and trauma may play a role in its development. Though it is not considered life-threatening, the condition can impact daily activities and overall quality of life. If you notice lumps or nodules on the bottom of your feet, it is suggested that you consult a podiatrist who can accurately diagnose and treat the condition.
A plantar fibroma may disrupt your daily activities. If you have any concerns, contact David K. Morris, DPM of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Plantar Fibroma
A plantar fibroma is a fibrous knot in the arch of the foot. It is embedded in the plantar fascia which is a band of tissue that extends from the heel to the toes along the bottom of the foot. There can be multiple plantar fibromas in the feet at the same time. There are no known causes for this condition. If you have a plantar fibroma, there will be a bump in the arch of your foot that cannot be missed. Any associated pain is most often due to a shoe rubbing against the nodule. Non-surgical options, such as steroid injections, physical therapy, and orthotics should be tried first. Surgery is a last resort and is the only thing that will remove a plantar fibroma entirely. Consult with a podiatrist for a proper diagnosis and to determine the treatment regimen that is right for you.
What Causes a Plantar Fibroma?
While there are no specific causes identified, a plantar fibroma can possibly come from genetic predisposition or the formation of scar tissue that forms from healing the tears in the plantar fascia.
What Are the Symptoms of a Plantar Fibroma?
There will be a noticeable lump in the arch of the foot that may or may not cause pain. If pain is felt, it is typically because a shoe is rubbing up against the lump or when walking or standing barefoot.
Treatment and Prevention
A plantar fibroma will not disappear without treatment, but it can get smaller and be a non-issue. If pain persists, a podiatrist examines the foot and when the arch of the foot is pressed, pain can be felt down to the toes. An MRI or biopsy might be performed to help diagnose or evaluate the plantar fibroma. The following non-surgical options are generally enough to reduce the size and pain of these nodules:
- Steroid injections
- Orthotics
- Physical therapy to help apply anti-inflammatory creams on the bump
Surgery is considered if the mass increases in size and the patient continues to feel pain after non-surgical methods are tried.
If you have any questions please feel free to contact our office located in Plantation, FL . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Relief Options for Ingrown Toenails
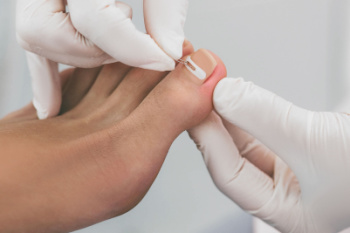
Ingrown toenails occur when the nails grow into the surrounding skin, leading to pain, redness, and possible infection. While mild cases of ingrown toenails can sometimes improve on their own, more severe or persistent cases often require medical care. A podiatrist can assess the severity of the ingrown toenail and offer specific treatment options. In advanced cases, minor surgical procedures, such as partial or total nail removal, may be necessary to alleviate pain and prevent recurrence. Ingrown toenails that become infected may also be treated with antibiotics, if needed. Early intervention can reduce the likelihood of such complications, especially for patients with diabetes or circulation issues. Regular care from a podiatrist, such as learning how to correctly trim nails and wearing shoes that fit properly, can also help. If you have a painful ingrown toenail, it is suggested that you schedule an appointment with a podiatrist for an exam and treatment.
Ingrown toenails may initially present themselves as a minor discomfort, but they may progress into an infection in the skin without proper treatment. For more information about ingrown toenails, contact David K. Morris, DPM of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails are caused when the corner or side of a toenail grows into the soft flesh surrounding it. They often result in redness, swelling, pain, and in some cases, infection. This condition typically affects the big toe and may recur if it is not treated properly.
Causes
- Improper toenail trimming
- Genetics
- Improper shoe fitting
- Injury from pedicures or nail picking
- Abnormal gait
- Poor hygiene
You are more likely to develop an ingrown toenail if you are obese, have diabetes, arthritis, or have any fungal infection in your nails. Additionally, people who have foot or toe deformities are at a higher risk of developing an ingrown toenail.
Symptoms
Some symptoms of ingrown toenails are redness, swelling, and pain. In rare cases, there may be a yellowish drainage coming from the nail.
Treatment
Ignoring an ingrown toenail can have serious complications. Infections of the nail border can progress to a deeper soft-tissue infection, which can then turn into a bone infection. You should always speak with your podiatrist if you suspect you have an ingrown toenail, especially if you have diabetes or poor circulation.
If you have any questions, please feel free to contact our office located in Plantation, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.